An insulin pump is an electronic device that connects to your body and allows for continuous delivery of small doses of insulin 24 hours a day based on a person's individual insulin requirements. An insulin pump functions like an artificial pancreas and is indicated for the management of type 1 and type 2 diabetes.
Insulin pumps use rapid- and/or short-acting insulin and are programmed to continuously release small quantities of insulin throughout the day, helping to maintain blood sugar levels within the normal range.
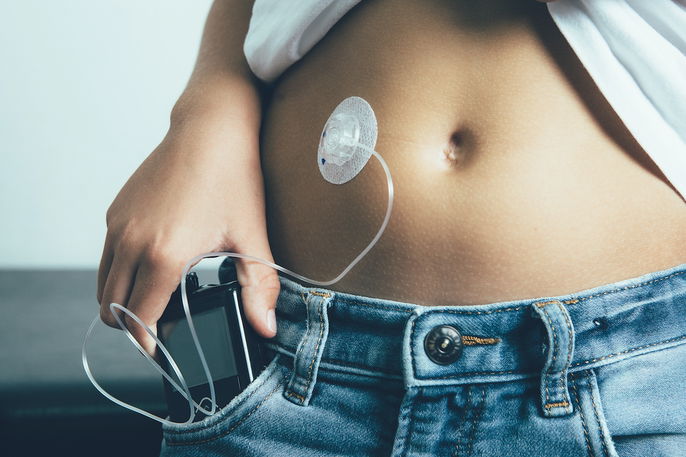
An insulin pump connects to the body through a small cannula (tube) containing a flexible needle that is inserted under the skin. They can be worn attached to the waist or upper arm. Insulin pumps should only be used under the supervision of an endocrinologist and requires teaching by a nurse or diabetes educator prior to use.
Reasons for use
Insulin pumps are indicated for the treatment of type 1 and type 2 diabetes when insulin production in the body is not sufficient to control blood sugar levels.
Insulin pumps are prescribed by an endocrinologist and require regular follow up to verify good blood sugar control and to make sure the person is adjusting well to using the pump.
Clinical indications
An insulin pump may be recommended in the following situations:
- Inadequate control of blood sugar levels due to difficulty with self-injections or forgetting doses;
- Large fluctuations in blood sugar levels during the day;
- Fasting blood glucose above 140 to 160 mg/dL (7.8 to 8.9 mmol/L);
- Frequent or severe episodes of hypoglycemia;
- Gestational diabetes;
- Planning to become pregnant.
Insulin pumps can also improve quality of life and may be a more comfortable option for the treatment of diabetes.
How it works
An insulin pump works by continuously delivering small amounts of insulin throughout the day and in the form of a bolus when necessary. Insulin is delivered through a small catheter that is inserted under the skin of the abdomen, upper arm, or thigh, which are the same sites used to inject insulin manually.
Insulin pumps are about the size of a small cell phone and are programmed to administer insulin as if it were a pancreas, allowing for better control of blood sugar levels.
It is also possible to use an insulin pump with continuous glucose monitoring (CGM) that checks blood sugar levels 24 hours a day and triggers an alarm when levels are very low or very high.
Care instructions
It is important to adhere to certain care instructions when using an insulin pump, including:
- Changing out the catheter every 2 to 3 days, with a small amount of discomfort to be expected at the insertion site;
- Washing your hands and the insertion site with water and a gentle soap every time you change the cannula;
- Alternating the insertion site of the cannula;
- Verifying blood glucose levels during the day, by means of a capillary glucose test (fingerstick) at least 4 times a day, including before each meal and at night before bed;
- Checking your blood sugar more frequently if your levels are more difficult to control. Your doctor may recommend checking your blood sugar 6 times a day (before and 2 hours after breakfast, lunch, and dinner) and also at night;
- Inspecting your skin at the insertion site, to take note of any localized inflammation, infection, or allergic reaction in the form of redness or swelling.
It is important to receive teaching prior to using an insulin pump, which is usually given by a nurse or diabetes educator.
Advantages to use
An insulin pump has the advantage of providing more accurate and precise amounts of insulin without the need for multiple daily injections.
Additionally, an insulin pump helps to better control blood sugar levels by providing a continuous delivery of insulin.
Possible complications
Complications that can occur while using an insulin pump include:
- Hyperglycemia;
- Hypoglycemia;
- Diabetic ketoacidosis (DKA);
- Infection of the skin at the insertion site.
Pump malfunctions, disconnection of the cannula, and incorrect pump settings can also interfere with the delivery of insulin and increase the risk of complications.
For this reason, it is important to receive adequate teaching prior to using an insulin pump in order to ensure it works properly and delivers the appropriate amount of insulin.
Where to buy
Insulin pumps can be purchased at medical supply stores or directly from the manufacturer and require a prescription from your doctor or other healthcare provider.
Insurance may cover the cost of an insulin pump but may have certain requirements. Make sure to check with your insurance company about coverage details and work with your healthcare team to choose a pump that is right for you.






























